Publications
![[Translate to Englisch:] [Translate to Englisch:]](/fileadmin/user_upload/Presse_und_Medien/mediathek/YouTube-Vorschaubild/NOA-Namur-Open-Architecture-Connectivity.jpg)
18.01.2018
Cardiovascular diseases are still the most frequent cause of death in Germany. Every fourth person dies of heart disease. Every year, around 1.71 million people are admitted to hospital for a heart disease.

This can be seen in the current annual report of the German Heart Foundation. Most of the heart diseases included in the report increased in 2016 compared to 2015 - in some cases significantly. For example, there was an increase of 4.2 percent in heart valve diseases, 2.6 percent in cardiac arrhythmias and 2.5 percent in heart failure. This is particularly worrying as the trend has been declining in the last two years. Heart diseases also remain dependent on regional factors or gender status. For example, the states with the lowest cardiologist density have an above-average infarct mortality rate. These include Brandenburg with a death rate of 83 (to 100,000 persons), Saxony-Anhalt with a death rate of 82, Thuringia with a death rate of 69 and Mecklenburg-Western Pomerania with a death rate of 68. Last year 117,518 women died of coronary heart disease, compared with 103,993 men.
Nevertheless, many patients are getting older with their cardiac insufficiency.
"State-of-the-art medical technology as well as innovative diagnosis and therapy procedures contribute to the fact that heart diseases can be detected earlier and treated even more effectively. All information and scientific findings relevant to the patient are consulted and used for his treatment," explains Christian Erbe, Chairman of the Medical Engineering Division (ZVEI). In future, this will also apply to data collected by medical devices at home, fitness trackers, health apps or other mobile data sources. According to Erbe, the digitalisation of the health industry thus leads to individualised health care oriented towards people's needs and living conditions.
In addition, digital technologies can make a major contribution, especially in emergencies. "Telemedicine serves as a kind of early warning system. The daily measurement of vital data enables early detection of the onset of hydrophilic decompensation, i.e. acute fluid overload and timely adjustment of the medication. This not only avoids emergencies: For patients, this preventive care provides a high degree of additional safety in everyday life and thus a considerably higher quality of life," continues Erbe. Also thanks to telemedical coaching, those affected learn to deal better with the disease and to behave more health-consciously.
In the healthcare industry, digitization and comprehensive networking in medical care make completely new methods and procedures possible. "In order to be able to implement them, however, we need reliable framework conditions for the financing of services and for the use of health data in care and research. Politicians must finally assume their responsibilities here. We need a common goal for the digitalization of the health industry", concludes Christian Erbe, chairman of the Medical Engineering Divisiond.
Practical example of the digital health economy: telemonitoring can help with heart failure
With telemonitoring it is possible to observe a patient with a chronic disease at home. The patient then no longer has to go to his family doctor for check-ups as frequently. Constant home monitoring also helps to reduce or even prevent critical situations and emergencies because a deterioration in health is noticed immediately. The attending physicians can thus quickly take the right treatment measures. Experts from other locations can also be called in and duplicate investigations can be avoided.
Around 1.8 million people in Germany suffer from cardiac insufficiency - and the trend is rising. But despite increasing numbers of cases, there are fewer and fewer deaths. Innovative, digital medical technology is one of the main reasons for this. Many patients with heart failure are carriers of an implanted defibrillator (ICD) or cardiac resynchronization device (CRT). These devices automatically transmitted information such as changes in the heart rhythm, shock releases or system function to a central data point via cellular services.

Easy-to-use measuring devices enable the patient to record important data about his or her state of health in everyday life. For example by a mobile ECG device or a blood pressure monitor. This gives him a direct overview of his state of health in everyday life. It is supported by an app, for example. At the same time, the data is forwarded to a telemonitoring office. All necessary measures are coordinated from there.
If the patient's measured values change suddenly and dangerously, this is immediately noticed in the telemonitoring centre, which is manned around the clock. The patient then receives a call or is contacted via a video connection. In this way, the patient receives instructions on how to behave and whether the centre must alert an emergency doctor.

In emergencies, the telemonitoring centre can directly alert the emergency service. On the way to the patient's home, the central office can then provide the emergency physician with further important information on current medication intake, existing allergies or the state of health in the last few days. This information helps the emergency physician to make the right decisions for the treatment of the patient more quickly on site.
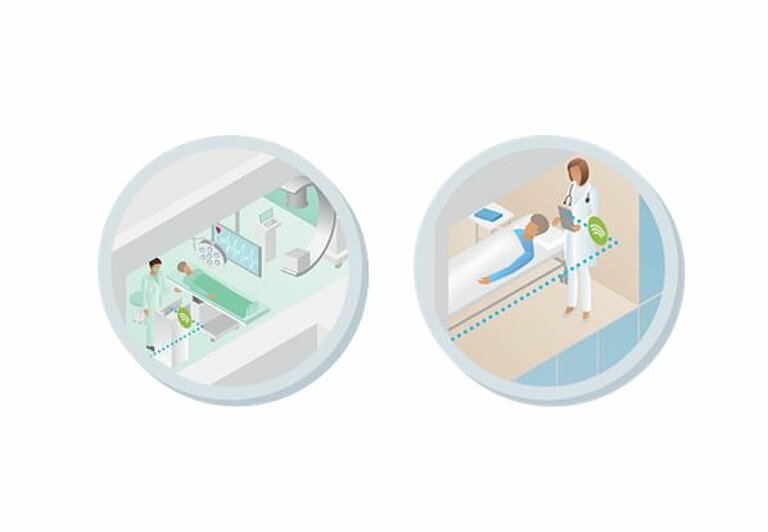
Information on the patient's medical history is particularly important for patients admitted to the clinic as an emergency. In the case of telemonitoring, the head office can provide this data to the hospital in which the patient is being treated. At the same time, the measures and data taken in the ambulance can be forwarded electronically to the responsible clinic in real time. In order to ensure high treatment quality throughout, additional experts at other locations can be consulted in real time via teleconsultations. Communication takes place, for example, in form of a video conference.
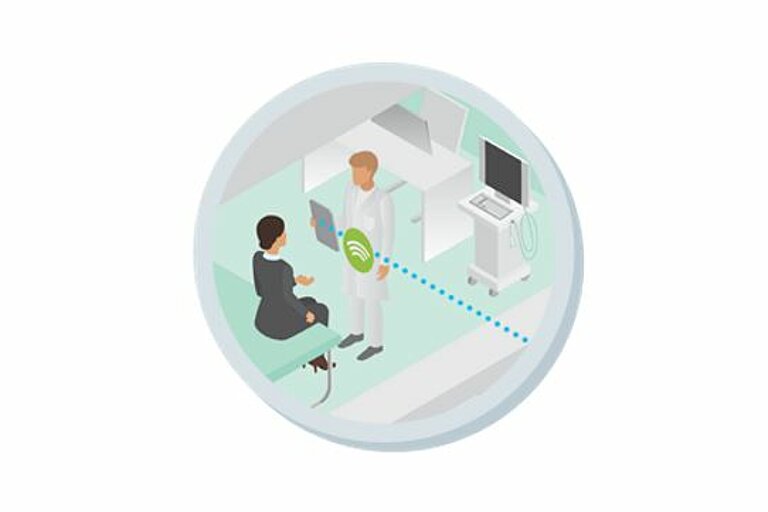
General practitioners and specialists must be able to exchange information about a patient's findings and treatment steps. This can be done, for example, via an electronic patient file.
With a telemonitoring solution, the patient regularly visits his family doctor for a thorough examination. The family doctor is provided with all relevant data and information since the last visit by the telemonitoring center. Because the patient has collected the same data every day, the family doctor has a much better picture of the patient's state of health at his disposal. Together with the patient, he can then determine the most suitable therapy for him. This can also be done through regular video consultations.
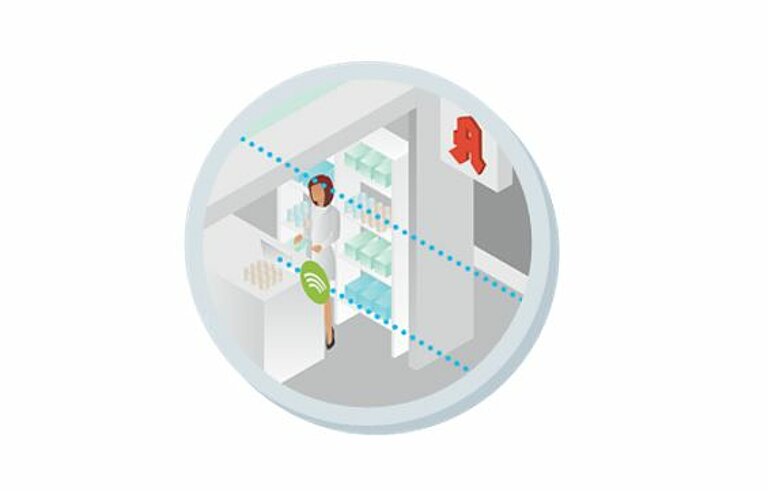
From 2018 on, every insured person can voluntarily have their medication plan stored on the electronic health card. It should contain as many prescription drugs as possible that the patient takes, as well as self-medication. Although the medication plan is prepared and updated by the family doctor or other physicians receiving treatment, pharmacists can supplement the plan at the patient's request with the medicines delivered to the pharmacy.

Personal telemedical coaching encourages the implementation of a more active and healthy lifestyle in everyday life. This has a positive effect on one's own health and quality of life and prevents concomitant and secondary diseases. Mobile applications (wearables and apps) can also help by collecting data that can be used in medical treatment and thus strengthen the areas of aftercare and prevention.

All medical data concerning the patients can be made available from the respective data sources on demand or online. Alternatively, the data can also be stored and managed in an electronic patient file. In this way, the necessary data can be made available to the practitioners. The patient decides who has access to the data. Special solutions can be agreed for emergencies.